Types of Varicose Vein Treatment
There are different types of varicose vein treatment. They include: Endothermal ablation, Sclerotherapy, and Surgical procedures, and each of these treatments have a distinct advantage. However, they are not suitable for all individuals. For this reason, choosing the appropriate type of treatment is critical.
Sclerotherapy
Sclerotherapy for varicose varices is a minimally invasive procedure. The procedure is safe and does not leave scars. However, it takes a few sessions to complete., and patients usually have to stay off their feet for several days following treatment. The doctor will then inject a sclerosant through a catheter. The procedure also eliminates the need for painful ligation.
The OdysseyVeinClinic Varicose Vein Treatment Adelaide procedure is used to eliminate unsightly varicose veins. It can also relieve the pain of nightly leg cramps. The treatment does not require surgery, and patients can resume normal activity afterwards. However, standing up right after the procedure is important to avoid potentially life-threatening blood clots.
Sclerotherapy can greatly eliminate varicose veins, as it can significantly reduce or eliminate their appearance. Patients can have this treatment at a clinic that specializes in this type of treatment. This doctor will perform this procedure at the Serene Radiance Laser Centre in Rutherford, and you can visit them for a consultation. Sclerotherapy involves injecting a sclerosant into the diseased vein, scarring the inside of the vein. After the procedure, patients can wear compression stockings to keep the area elevated and minimize pain.
Sclerotherapy is a quick procedure that can be done as an outpatient procedure. After the procedure, patients can resume normal activities, but avoid strenuous activities for a few days is recommended. Mild bruising and discomfort should subside within two to six weeks. Patients can also wear compression gear to promote circulation and blood flow.
Another OdysseyVeinClinic Varicose Vein Treatment Adelaide is mechanochemical endovenous ablation (MOCA). In this treatment, a catheter is inserted into the vein, where a sclerosant is delivered to the affected vein. The distal end of the catheter contains a balloon, which temporarily blocks blood flow to the targeted vein segment. However, the safety of endovenous catheter-directed chemical ablation is not yet well-established in the medical community.
Although sclerotherapy for varicose veins does not permanently eliminate the symptoms of varicose veins, it is a very effective alternative to surgery and other treatments. It is safer, less invasive, and has an 80% success rate. Aside from reducing pain and improving veins’ appearance, sclerotherapy is more cost-effective than surgical procedures.
Sclerotherapy for varicose venous disease is not without risk. Several complications may occur, including numbness, swelling, and redness. Patients should discuss their medical history and any side effects with their physician before undergoing a procedure. The results of a study can help patients decide which procedure is best for their situation.
Endothermal ablation
Endothermal ablation is an excellent treatment for many types of varicose veins. The procedure is usually performed under a sedative but can also be done under general anesthesia. This procedure injects salt water and anesthetic agents into the vein. Then, the surgeon inserts a catheter into the vein to be treated. The vein is typically located below the knee, although this may occasionally be performed on the ankle.
The endovenous thermal ablation procedure is usually very safe, but it does carry risks. Possible side effects include bruising or pain at the site of the treatment. The procedure may also cause vein scarring. You should be aware of these risks and discuss them with your physician.
Another OdysseyVeinClinic Varicose Vein Treatment Adelaide is endovenous laser ablation, which is a minimally invasive option to stripping. This procedure is best for people with large saphenous varicose veins. These veins must be at least 4.5mm in diameter.
There are several options for endothermal ablation. Endolaser (EVLA, ELVS, and ELAS) is a patented treatment for large varicose veins. It is FDA-approved and has a high success rate of 97%. The procedure will involve a small cut in the vein to deliver high-frequency radio waves to the underlying tissue.
This treatment is often performed by vascular surgeons or pain management clinicians. The procedure is less invasive than traditional surgery, and patients can return to normal activities soon after. In addition, using tumescent anaesthesia avoids the risks of spinal or general anesthesia.
This procedure can improve the quality of life of a patient with severe varicose veins. It is an outpatient procedure with minimal recovery time and little to no side effects, and this treatment can also help reduce the risk of a patient experiencing complications.
The treatment is also a good option for patients who have failed conservative management. It is best performed on patients with symptomatic varicose veins at least six mm wide. In some cases, endothermal ablation may be accompanied by ultrasound-guided sclerotherapy.
Surgical procedures
There are several surgical procedures available for the treatment of varicose veins. Some involve the use of radio waves or lasers to collapse the vein. These procedures are minimally invasive, and the patient is usually awake during the procedure. Some involve the use of small hooks or needles to puncture the skin.
Surgical procedures for varicose veins can involve an incision in the skin. The sclerotherapy procedure can be performed with or without ultrasound guidance. This procedure causes the vein to scar, which forces blood to reroute through healthy veins. Once the vein becomes scarred, it eventually collapses and is absorbed by the body.
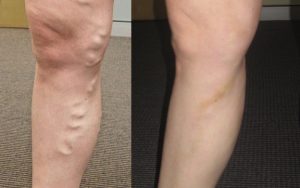
Varicose veins can occur anywhere on the body, but they are most common in the legs. These large protruding veins are usually unsightly and can cause significant discomfort. In addition, they can lead to chronic wounds, blood clots, and severe skin changes if not treated.
Surgical procedures for varicose veins can have many risks, including wound infections, pain, swelling, and skin discolouration. However, these risks are relatively small, and most patients return to normal life after the procedure. After a successful treatment, 80% of patients report improved symptoms and appearance.
Surgical procedures for varicose veins are usually performed under general anaesthesia. The physician inserts a catheter through the skin to inject a medical adhesive into the varicose vein. They then press on the vein to close it. After this procedure, blood returns to the healthy veins nearby. The procedure usually takes less than an hour and can be performed by a vein specialist.
Before varicose vein surgery, a patient will undergo various tests to assess their condition’s severity. This test will determine whether or not a patient is a good candidate for the procedure. The doctor will also check the condition of the veins and recommend any treatment options.
Surgical procedures for varicose vein treatments are performed to reduce pressure on the veins in the legs. It prevents new varicose veins from growing or enlarging. It also minimizes the risk of further skin ulceration surrounding the ankles.
 Surgical procedures for varicose veins may include lasers, radiofrequency, or radio waves to close veins. This procedure is minimally invasive and requires less local anesthesia than thermal treatments. The doctor inserts a small tube called a catheter into the affected vein. The catheter is then threaded through the vein, and a clot-dissolving liquid is injected. Surgical procedures for varicose vein treatment are often performed on an outpatient basis. However, some patients may be admitted to the hospital after the procedure, so it is important to ask your doctor for additional information.
Surgical procedures for varicose veins may include lasers, radiofrequency, or radio waves to close veins. This procedure is minimally invasive and requires less local anesthesia than thermal treatments. The doctor inserts a small tube called a catheter into the affected vein. The catheter is then threaded through the vein, and a clot-dissolving liquid is injected. Surgical procedures for varicose vein treatment are often performed on an outpatient basis. However, some patients may be admitted to the hospital after the procedure, so it is important to ask your doctor for additional information.
Another surgical procedure for varicose vein treatment involves hooks to remove the veins. The procedure is often combined with an endovenous procedure but can be performed alone. It will leave a small incision and is often an outpatient procedure. Scarring is usually minimal.